Neck pain is a serious problem in a person’s life that is hard to ignore, as it limits you in your daily activities and tasks.
Neck pain is described as an unpleasant sensory and emotional experience caused by biological (tissue damage) or psychological factors and, in some cases, extends to the shoulder area and down the arm to the fingers.
Neck and back pain are called a multifactorial disease because it is caused by various risk factors such as degenerative changes in the spine, herniated discs, cervical spinal stenosis, lack of physical activity, excessive use of the computer and telephone, the impact of stress, emotional distress, anxiety, old age and low social support. Early detection of risk factors and triggers of neck pain leads to more effective diagnosis, treatment and pain management (6).
Anatomy and origins of neck pain
The neck is the main support for the head and is its connection to the rest of the body. Anatomically, it is located between the lower jaw and the clavicle. Contains the most compact and numerous vital structures essential for the normal physiological functioning of the human body. Anatomical structures in the neck allow the functions of breathing, speaking, swallowing, metabolism, brain-spine connections, circulation and lymphatic inflow and outflow from the head to function smoothly. (3).
The cervical spine is made up of 7 vertebrae that are anatomically positioned one above the other. The vertebrae are interconnected and form the spinal canal, which is the passageway for the spinal cord and its nerves. The main function of the spinal cord is to transmit messages (sensory and motor impulses) between the brain and the rest of the body. Between the vertebrae are the intervertebral discs, which are made up of a hard and flexible outer ring (called the annulus fibrosis) and a soft central disc (called the nucleus pulpous). The intervertebral disc distributes the impact of mechanical forces generated on the spine during everyday life (gravity, physical activity, etc.). (1).
Types of neck pain
Neck pain is classified according to the duration of the problem (acute phase lasting up to 6 weeks, sub-acute phase lasting 3 months or less, chronic phase lasting 3 months or more), the severity of the pathology, the type of aetiology (the type of cause of the problem) and the type of pain (mechanical or neuropathic pain).
Neck pain can be mechanical, neuropathic or secondary in origin. Secondary or other causes represent pain from the heart, vascular pathology or referred pain from adjacent anatomical structures.
Mechanical pain originates in the spine or its supporting structures (ligaments, muscles) and manifests as arthritis, discogenic pain and myofascial pain. Mechanical pain typically worsens during movement.

Neuropathic pain occurs as a result of injury or disease of the nervous system and is divided into central or peripheral pain. The main symptom of neuropathic pain is burning pain in the neck.
Central neuropathic pain is caused by the spinal cord and manifests as symptoms of myelopathy (disturbed motor and sensory impulses). Peripheral neuropathic pain is caused by peripheral nerve damage and is recognized as radicular symptoms resulting from herniated discs, osteophytes (bone growths) or spinal stenosis.
NECK PAIN RATING SCALE
| DEGREE OF NECK PAIN |
DESCRIPTION
|
|
LEVEL I.
|
Neck pain with minimal or no interference with activities of daily living.
|
|
LEVEL II.
|
Neck pain that limits your daily activities.
|
|
LEVEL III.
|
Neck pain spreading to the arm (associated radiculopathy/”pinched nerve” – burning pain in the neck, weakness and numbness in the arm)
|
|
LEVEL IV.
|
Neck pain caused by serious pathology (tumour, fracture, infection, systemic disease).
|
WHO IS MOST OFTEN AFFECTED BY NECK PAIN?
Neck pain affects women more often than men.
Risk factors for pain include genetics, psychopathology (depression, anxiety, catastrophising, etc.), sleep disorders, smoking and sedentary lifestyle.
Obesity has been shown to be a major contributor to neck pain, as individuals with increased body weight are more prone to systemic inflammation, adverse structural changes, increased mechanical stress, reduced muscle strength and more prone to psychosocial problems.
Neck pain is caused by trauma (brain injury, neck injury) or a sports injury (wrestling, boxing, ice hockey, etc.).
Some studies have shown that office, computer, manual and healthcare workers are more prone to neck and back pain. A poor working environment and low job satisfaction have a significant impact on the development of neck pain (2).
5 pathological causes of neck pain
The most common disorders of the neck and occipital region are cervical spine sprain and strain, cervical osteoarthritis, degenerative disc disease, cervical radiculopathy, stiff neck (german: hexenschuss), and herniated discs. A more detailed description of the diseases is given below.
1. Cervical spine oscillatory injury
A swinging neck injury usually occurs as a result of a car accident, sports injury or fall, where there is a sudden movement of the head from hyperextension (head direction: extreme rearward gaze towards the ceiling) forward into flexion (head direction: gaze towards the ground). In some cases, the spinal injury indirectly affects the joints or discs that irritate nerve roots and nerves.
Individuals with symptoms of whiplash report neck pain and stiffness, radiating pain in the shoulders or back, numbness and tingling of the entire upper limb, headaches, dizziness, sleep disturbances, or vision problems (blurred vision, sensitivity to light, etc.).
A swing neck injury is a cluster of clinical signs that lead to a medical diagnosis, such as a neck strain or sprain (4).
2. Difference between a strain and a sprain
A neck strain is defined as a strain of a muscle in the neck or an injury to the tendon of a muscle (the fibrous tissue that connects the muscle to the bone), while a sprain is a tear of the ligament (the fibrous connective tissue that connects two bones) that interconnects the cervical vertebrae.
Poor posture, inappropriate sleeping positions, sudden neck movements (car accident, sports injury, fall) all contribute to neck strain or neck sprain.
Individuals experience pain and stiffness in the neck on movement, radiating pain in the upper shoulder, reduced neck mobility and the onset of muscle spasms (4).
3. Cervical osteoarthritis, degenerative intervertebral disc disease and cervical radiculopathy
Cervical osteoarthritis, or cervical facet joint syndrome, is a degenerative condition of the cervical spine in which the cartilage in the facet joints wears away. Often the degeneration of the facet joints affects the degeneration of the intervertebral discs, which in turn leads to nerve root compaction (symptoms of radiculopathy).
Symptoms of cervical osteoarthritis are stiffness and pain in the neck, localised in one place (point pain), less often radiating to the shoulder or back of the head.
Cervical osteoarthritis occurs as a degenerative process of ageing, neck injury or overweight.
Ageing is a natural evolutionary process that causes wear and tear changes to occur in the intervertebral discs of the cervical spine. Individuals with degenerative disc disease experience neck pain and stiffness, which worsens with movement.
Treatment of degenerative intervertebral disc disease in the cervical spine depends on the degree of symptom severity and the presence of neurological symptoms.
Surgical treatment is necessary in long-term cases, in the presence of neurological symptoms.
Degenerative changes lead to narrowing of the intervertebral space and the formation of bony growths that pinch the nerve root, called cervical radiculopathy.
Cervical radiculopathy is felt as pain and tingling from the neck down the entire upper limb and increased weakness of the neck and upper thigh muscles.
Nerve root compression is caused by spondylosis (degenerative changes), osteophytes (bone growths), instability of anatomical structures, traumatic injury, or tumour.
A pinched nerve root causes problems with walking, balance and bladder or bowel dysfunction (6).
4. Stiff neck
Neck pain is usually caused by muscle tension or a joint condition in the cervical spine (osteoarthritis, injury to the facet joint). A stiff neck occurs after lifting a heavy load or, more often, while sleeping in an inappropriate position.
The main symptom of a stiff neck is limited range of movement of the cervical spine or difficulty moving the head. The stiffness occasionally leads to muscle pain or nerve compression, which is felt as a burning pain in the neck and a tingling sensation throughout the upper limb. (2).
Symptoms of a stiff neck can be treated in home care through pain relief and improved range of motion in the neck. Ice (cryotherapy) is recommended for the first three days after the neck stiffness, as this reduces inflammation and pain. In the following days, apply heat (thermotherapy) to increase blood flow to the neck area and reduce stiffness.

You can improve the management of the main symptom of stiff neck, limited range of motion, with appropriate stretching and range-of-motion exercises. It is advisable to avoid movements that further trigger pain.
5. Can a hernia be in the neck?
Herniated discs occur from the cervical to the first sacral spinal vertebra. A herniated disc occurs when the soft centre of the intervertebral disc (nucleus pulposus) bulges and compresses the nerve root.
Symptoms of a herniated disc take the form of radiculopathy (nerve root compression), which individuals describe as a burning pain in the neck or a sensation of electricity spreading from the neck down the arm to the fingers. Herniation symptoms include a tingling sensation in the arm, hand, fingers, weakness of the neck muscles and the muscles of the entire upper limb.
Herniated disc is diagnosed by an appropriate diagnostic examination and physical examination. To further confirm the diagnosis of a herniated disc, an imaging diagnostic method called magnetic resonance imaging (MRI) is recommended.
Adequate diagnostic screening and special physiotherapy rehabilitation drastically reduce the chance of surgery (cervical discectomy) to remove the herniated disc (7).
When do I know if neck pain is dangerous?
Neck pain is dangerous when it occurs as a result of a traumatic injury or when symptoms of headache, fever, nausea, vomiting or shortness of breath are present.
How can we reduce burning pain on our own?
Here are ways you can reduce the burning pain in your neck and improve your quality of life.
Avoid sitting for long periods of time, or make time for movement in your sitting routine to stretch, stretch and exercise (to limit the effects of poor posture).
Follow ergonomic tips when using your computer and phone (ideally set at eye level).
Organise your sleep routine accordingly to ensure your body gets enough sleep (use a suitable pillow for the most optimal neck alignment when sleeping) (5).
At MedicoFit, we recommend self-massage of tight neck muscles to relieve pain and the correct neck pain exercises to strengthen the neck muscles.
Physiotherapy diagnostic examination for neck and occipital pain
The diagnosing physiotherapist will use your medical history, the history of your symptoms and the etiology of your problem to appropriately determine the origin of your primary neck pain. Further determined by the duration of the problem as acute neck pain often becomes chronic. Through the diagnostic process, it distinguishes possible referred neck pain from pathologies that require specific treatment, such as thoracic outlet syndrome, upper limb pain, vascular pathology and pain from the thoracic viscera (heart, lungs).
Through physiotherapy diagnosis, it is important to distinguish neuropathic from mechanical pain, which in turn influences decisions on further treatment. Neuropathic pain, which can arise as a result of spinal stenosis or disc herniation, is described by individuals as a stabbing, electric and burning pain in the neck, radiating to one or both upper limbs. Mechanical pain, unlike neuropathic pain, is more throbbing and sharp.
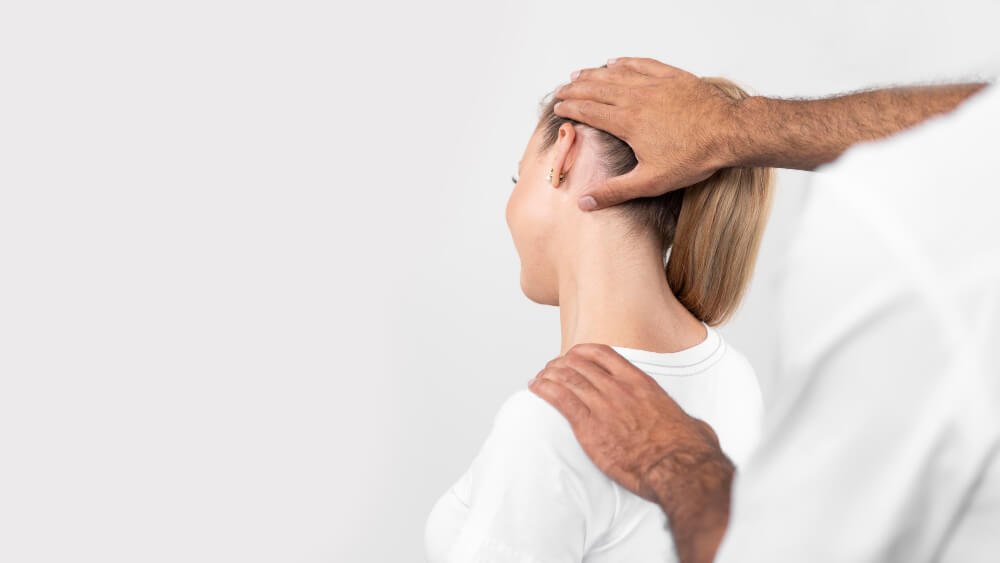
The physiotherapy diagnostic process includes a physical examination, where the diagnostic physiotherapist checks your neck range of motion, muscle strength, identifies any muscle imbalances, sensory sensitivity, posture, spinal movement pattern analysis and functional mobility.
An important diagnostic factor is the cervical spine’s load-bearing capacity, which provides an estimate of its load-bearing capacity.
Based on all the information gathered about your condition, a specialized individual physiotherapy programme is developed.
Book your diagnostic appointment now!
Special physiotheraphy at Medicofit clinic
The effectiveness of specialist physiotherapy differs from passive treatments such as rest in its focus on individualised kinesiotherapy, i.e. active exercises and postural correction in the treatment of neck pain. Rest is recommended, but in reasonable proportion to your activity.
In the initial phase of individual physiotherapy, a diagnostic physiotherapist will assess the type of pain you are experiencing (neuropathic/mechanical) and, based on the findings, tailor an individual kinesiology programme aimed at reducing neck pain, possible nerve irritation i.e. pain and tingling radiating to the upper limb, and increasing the weight-bearing capacity of the cervical spine.
Individual kinesiotherapy is based on your diagnostic results, which have given us insight into your neck range of motion (which, if limited, is increased with flexibility exercises), any muscular imbalances and weaknesses of individual muscles/muscle groups (which are appropriately strengthened initially with isometric exercises, and in the next phase with counter-resistance exercises), which is why the programme is tailored specifically to your individual needs.
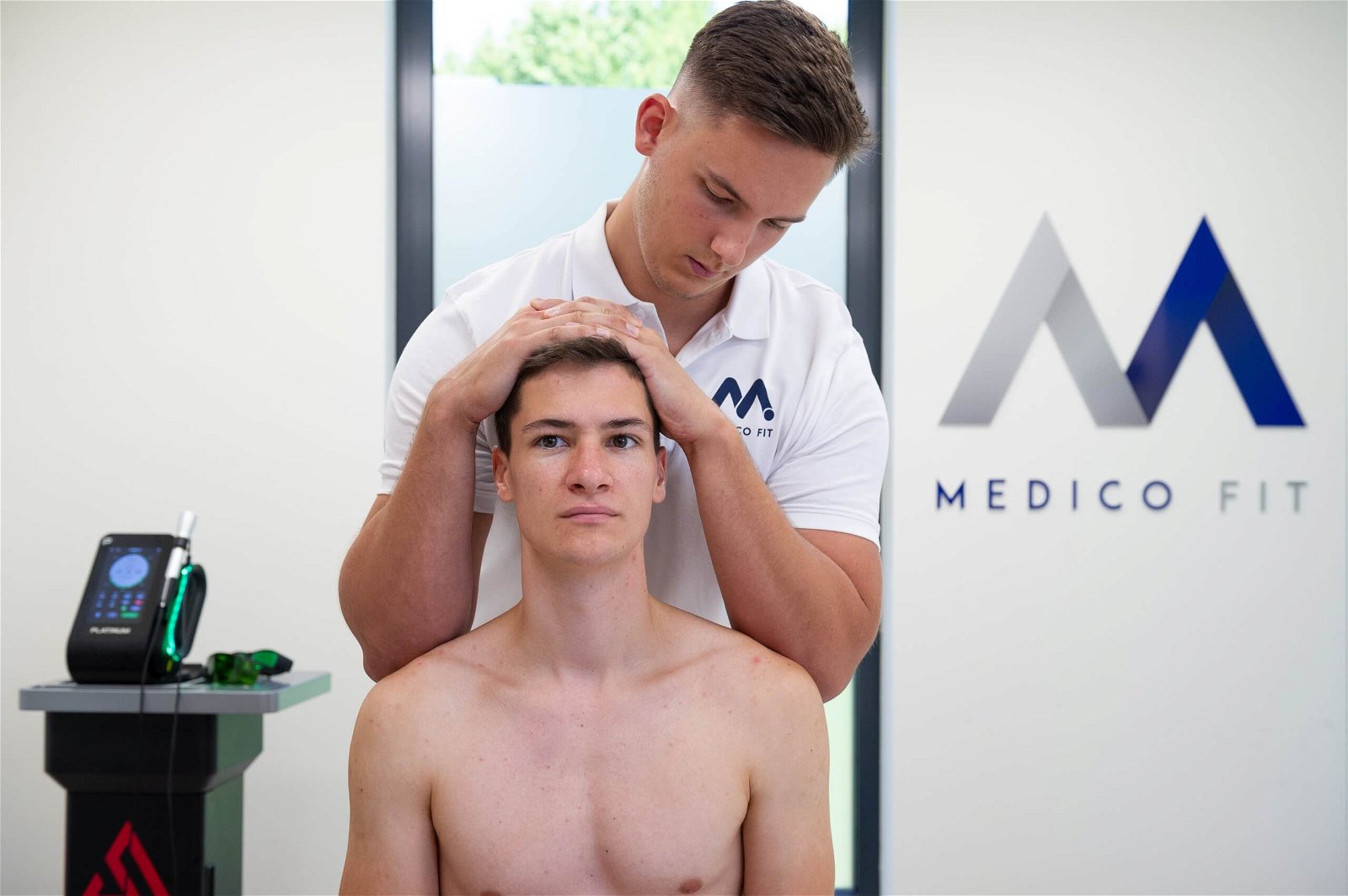
Analysis of postural movement patterns gives an in-depth insight into the dynamics of your spine and any deviations from the norm. To correct the posture and movement patterns of the spine, we initially focus on performing activation exercises for the cervical spine muscles, which are key to postural control. We continue with active exercises that first aim to establish the correct loading capacity of the cervical spine (full range of motion and strengthening in all directions of movement in the neck – flexion, extension, later flexion and rotation) and, once the results are achieved, focus on increasing the loading capacity of the cervical spine.
Active rehabilitation is crucial for a successful treatment outcome, but the latest physiotherapy assistive technologies such as HiTOP electrotherapy, LASER therapy, ultrasound therapy and PERISO therapy help us to achieve optimal results.
Eliminate neck pain for good
Neck pain negatively affects the functionality of your daily tasks and activities. The first step to successful problem solving is a professional diagnostic examination, which is a prerequisite for setting up an individual specialised physiotherapy programme.
The main purpose of modern physiotherapy rehabilitation for the long-term elimination of neck pain is a holistic approach involving interprofessional cooperation between medical, physiotherapy and kinesiology professionals, with a common focus on improving physical function and, consequently, your quality of life. This is the modern reality that MedicoFit clinic experts offer you today!
- Kelc R., 2012. Funkcionalna anatomija hrbtenice. VIII. Mariborsko ortopedsko srečanje. Interdisciplinarno strokovno srečanje. Hrbtenica v ortopediji. Zbornik predavanj. Maribor, pp. 13-23
- Cohen S. P. (2015). Epidemiology, diagnosis, and treatment of neck pain. Mayo Clinic proceedings, 90(2), 284–299. DOI
- Roesch ZK, Tadi P. Anatomy, Head and Neck, Neck. [Updated 2022 Jul 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: NCBI
- Bragg KJ, Varacallo M. Cervical Sprain. [Updated 2022 Sep 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: NCBI
- 6 ways to ease neck pain – Harvard Health. (2015, April 25). Harvard Health. Retrieved October 19, 2022.
- Kazeminasab S, Nejadghaderi SA, Amiri P, Pourfathi H, Araj-Khodaei M, Sullman MJM, Kolahi AA, Safiri S. Neck pain: global epidemiology, trends and risk factors. BMC Musculoskelet Disord. 2022 Jan 3;23(1):26. doi: 10.1186/s12891-021-04957-4. PMID: 34980079; PMCID: PMC8725362.
- Sharrak S, Al Khalili Y. Cervical Disc Herniation. [Updated 2022 Aug 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: NCBI